| GUEST BLOG |
The Privileges and Burdens of the Granddaughter Caregiver
Barry Jacobs, November 2018
Becky’s strong-willed grandmother, Patricia, steadfastly refused help from all family members — except from Becky. Her oldest grandchild, 26, had always been her favorite, and she still responded tenderly to her even as she reacted sourly to her own son and daughter, Becky’s mom. Only Becky received a big smile whenever she visited Patricia’s small apartment. Only Becky could convince her to take all her medications. Only Becky could cajole her to regularly use her walker and bathe.
Becky felt privileged — and burdened — by her special role. She loved her grandmother and enjoyed spending time with her. But she felt guilty, as if she were complicit, whenever Patricia rebuffed her mother’s pleas to consider hiring help. And she felt strained by the pressures of running errands for her grandmother and working a demanding full-time job. As the juggling became harder for her, she turned to her mother and uncle for help. The coolness of their responses spoke volumes. She realized they were envious that she got the best of their mother while they were dismissively held at arm's length.
As a large segment of millennial caregivers, caregiving granddaughters such as Becky are becoming more common. In many ways, they represent one of the most joyous and loving aspects of family life — a reaching across the generations to nurture one another. But granddaughter caregivers also have an ambiguous role. They can be helpful and persuasive but are not generally accorded the respect or authority of spouses or adult children by other family members. They are also often at a point in their own personal development when they expect to be focusing on their own growth, not an older relative’s decline. And, as in Becky’s case, they can be regarded by other family members with ambivalence.
How can granddaughters best employ their special relationships with grandparents who need help? And how can families best utilize those granddaughters to become valued members of the caregiving team? Here are some ideas:
Supplement, don’t supplant: It can be flattering to be the person in the family whom a loved one has preferentially selected to be the one and only primary caregiver. But being the lone hero, rather than a member of a crack caregiving team, can be wearying and alienate you from others who feel sidelined, denigrated and disenfranchised. That’s what often happens to granddaughter caregivers. They would cope better in the long run by sharing the glory. Their role would be clearer and more sustainable if they supported a grandparent’s adult children and let them assume the lead and the major responsibilities.
Respect your elders but set limits: Adult children have often gone through a period of adolescence and young adulthood during which they learned to assert themselves with their parents rather than forever jump to their every command. When the time for caregiving comes, they are hopefully able to have adult-to-adult negotiations with them about important decisions. Granddaughters — even those in their 20s and 30s — may have never forcefully expressed their own mind to a grandparent and may be deferential to a fault. But not every one of a grandparent’s wishes is wise nor preferences prudent during the caregiving years. It would be better for granddaughters to learn to push back — gently — at times to protect themselves from unreasonable demands or a grandparent from poor choices.
Exercise earned authority: It can be extremely frustrating for a granddaughter to contribute to a grandparent’s care but then be treated like a kid with little voice in the family deliberations about the grandparent’s present and future. If she is capable enough to handle crucial responsibilities and be relied on for her persuasive powers, then she merits having her perspectives heard. Caring well for a grandparent should be a way of earning due respect from a parent.
Be the legacy: One reason why grandmothers favor granddaughters is that they see themselves as they once were in them. They also see living evidence that their progeny and values are thriving in the world. Being that legacy — especially the smart, kind and hardworking sort — is as important a gift that a granddaughter can give a fading grandparent as laughter, good company and hands-on care.
Cherish the memories: Many caregiving granddaughters go about their sometimes difficult business with a sense that time is limited and that they’ll cherish these moments with their grandparents now as well as much later. Many care-receiving grandparents feel that way, too. The interactions between them, however mundane, then takes on a special meaning for a special relationship. Few granddaughter caregivers will ever look back with regret.
Barry J. Jacobs, a clinical psychologist, family therapist and healthcare consultant, is the co-author of the book AARP Meditations for Caregivers (Da Capo, 2016). Follow him on Twitter @drbarryjacobs and on Facebook.
|
The Key is Compassion – A Series
One Simple Practice So You Thrive in Every Area of Your Life
Virginia Sampson, September 2018
The key to thriving in life may surprise you; I know it did for me.
In 1993, when our youngest child was two weeks old, my husband was diagnosed with ALS (Lou Gehrig’s Disease). I became my husband’s full-time caregiver for three years while parenting three teenagers and a toddler. It was a challenging time in my life to say the least. Many people empathized with the difficult circumstances. However, very few showed any compassion.
You see, there is a difference between empathy and compassion. Empathy is present when someone feels or identifies with the pain or suffering of another. “I feel your pain,” we often say to someone experiencing death, illness or any type of suffering. This demonstrates our care, we say to ourselves. After all, we have no idea what else to do or say. Those tragic events are uncomfortable and even terrifying to confront in conversations with another. We simply want to escape the situation so we throw out a simple yet empty statement. But we forget, perhaps, that those who are experiencing those traumas do not get to escape.
Please don’t misunderstand me. Empathy is very, very important. However, at times it may not be enough. Often what we need to offer our friends is compassion. When you are compassionate you are empathetic (i.e. you feel the pain or suffering of another) AND you help alleviate that suffering with some form of action. It can be something simple. You can:
Bring a meal
Call and listen as they talk
Stop by, without pity, for a short visit
Help with some of their daily chores for which they no longer have time or energy
Send a message that you care
While caring for my husband, I stopped working. I didn’t leave the house except to “manage” the children. Some people would offer me sympathetic looks or even say how sorry they were to hear about my plight. Sadly, other people simply avoided me. However, no one really offered to do anything to help the family, and this included simply being kind to my children who were acting out the grief and pain of watching the devastating deterioration of their father every single day. For someone going through a very challenging time, empathy is greatly appreciated but compassion is essential.
I didn’t realize that at the time. It wasn’t until much later that I identified compassion as being missing from my life. I just knew no one was helping us. In our super busy lives and in our impersonal world, we can forget that the most meaningful parts of our lives are our personal connections. Empathy can be fleeting and quick, while compassion requires effort and time. It is compassion that creates meaningful connections.
For that reason, and many others, compassion helps us thrive. This discovery is the result of much research that has been and is being conducted at universities all around the world including UC Berkeley and Stanford University.
Dictionary.com defines “thrive” as to “grow or develop well or vigorously, prosper, flourish.” Researchers are establishing that with compassion, our schools, our businesses, our communities, our families and even our health all thrive.
Compassion helps us thrive, in part, because we are biologically and genetically programmed to be compassionate. For many years now, we have operated on the premise that Social Darwinism’s “survival of the fittest” governs our behavior and biology. In other words, the theory says we are by nature selfish, individualistic and competitive. However, researchers have been dispelling that notion. Instead, they have found that behaviors like compassion and kindness are rooted in our behavior and biology. They are actually conducive to human survival and essential to human flourishing.
My family went through the trauma of my husband’s painful decline and death essentially alone. As his body deteriorated, fewer and fewer people came to visit until, at the end, no one came to visit except his sister and her husband. The lack of visitors was perhaps even more painful to my husband than the loss of use of his body. You see, with ALS the person remains intact mentally as they lie trapped in a dead body. Some people call it “the coffin disease.” He was discarded even before he was dead. Compassion could have changed that.
Being compassionate feels good. There is biological evidence to support that when we give to others, it actually activates some of the pleasure centers in our brain. When we show compassion, we are tapping into our evolutionary nature and our biology.
In our society, we tend to see compassion as a touchy-feely emotion best relegated to our church lives or our volunteer activities. This new science has recognized the inaccuracy of that assumption. Compassion should be and must be an essential part of our individual lives, our schools, our communities, our business and our world if we are to thrive.
It must be the case, as well, if we are to survive.
|
Planning for the Ultimate Act of Love
Jon Braddock, August 2018
As I sit to write this article I struggle with where to begin. The title I have chosen seems huge since I’ve included the word ultimate! Yet my eyes focus on two other words, act and love.
It brings me to that old saying, “actions speak louder than words”.
To me this says what I do (act or action) is ultimately more important than what I say.
As I apply this to love, I can tell my wife numerous times a day that I love her, but are my actions supporting my words? Don’t get me wrong, the spoken word is important, but what about when I know longer have a voice? That leaves only actions. What do I want the experience to be like for my family after I have died? What will I do or what action will I take to ultimately show my family that I loved them so much, I wanted to ease their burden?
For me the ultimate act of love is planning ahead.
I call it Death Etiquette™
**********
Death Etiquette™
Being thoughtfully prepared for one’s own passing. Accordingly, making things easier for family and loved ones by leaving clear and concise instructions in regard to your final wishes for funeral desires as well as location and access to important documents and accounts. Further identifying who should be responsible for carrying out the final wishes and ultimately settling all the final affairs. It is a simple act which saves loved ones
Stress, Time and Money…. the things which divide families!
**********
I can’t imagine leaving my family scrambling for answers. Likely having to deal with months, if not longer, tracking down my documents, my accounts, and trying to close out all of the final affairs. Will they know what my funeral desires are? Will they be able to locate my Will, my insurance policies and all of my financial accounts? Do they know who my attorney and accountant are who will be able to assist them? Will they know how to access all of my online accounts from bill pay, pre-set auto drafts, and everything else from my Amazon account to all my social media accounts? Will they be able to unlock and access my computer, my tablet and my smart phone where I have so much valuable information stored? Will my children come to blows over who gets my watch, the china, the household furnishing and all my other stuff?
The sadness and grief of losing a loved one is enough hardship. I certainly don’t want to add frustration, confusion, stress, anxiety and anger to the list.
The good news is these things are easily avoidable by simply planning ahead.
So why don’t we?
Well I believe that for many of us we feel overwhelmed at what appears to be a daunting task. But it needn’t be if we tackle it logically. I like using a weight loss analogy. For example, if I want to lose 10 pounds, I can’t just wake up tomorrow morning and be 10 pounds lighter. That’s not realistic. Just like I can’t get all my planning done by tomorrow morning. It simply can’t be done that fast.
We have to look at it as a process.
Back to weight loss. If I say I will loss 10 pounds in the next 8 weeks, this becomes a very achievable goal. A little bit every day and each week doing the right things and 8 weeks from today, I will wake up 10 pounds lighter than I am today. BOOM, very doable!
I am hopeful you can see where I am headed. So, as it relates to planning. If I say I will have my planning done in the next 8 weeks, this also becomes a very achievable goal. Not so daunting or scary when I give myself some time. If I gather, sort and organize a little bit each day and each week, 8 weeks from today my planning will be done! BOOM, very doable!
Here are tips to get started.
Must Do:
Make your funeral wishes known (burial or cremation, wake or no wake, etc.)
Provide as much information as possible regarding financial accounts, such as life insurance policy numbers and beneficiaries, bank account numbers, safe deposit box locations, proof of ownership documentation, etc.
Provide a list of your advisors. Attorney, accountant, financial & spiritual.
Create a list of things you own and expenses.
Create a list of all online accounts, social and otherwise including, user name, passwords, and challenge questions.
Indicate how to access all of your technology, computers, tablets and smartphones.
Have a plan to close your social media accounts.
Be sure to update your beneficiary information.
State healthcare advance directives, so you have a voice when you can no longer speak.
Name a healthcare POA. Someone to act on your behalf I you are unable.
Tell someone you trust—your spouse, your most responsible child, a trusted friend, or legal representative—where to find your stuff, in particular the location of a document that clearly tells people what to do and where to go for it all.
Should Do:
Create a Will (move this one to the “Must Do” category if you have children).
Create a trust for your minor children, if applicable.
Periodically review your Will and beneficiary information.
If you have pets, name who should be responsible for their continued care.
Designate who gets which items (your stuff) to avoid potential family conflict.
Make a list of causes and charities you wish to donate to after your passing.
Pre-plan for funeral and memorial services.
And most importantly after you have completed your planning, keep it up to date! Things change and when they do, document it. It only takes a minute which could save your family hours.
For me, having been through this process and now having a plan in place, it has resulted in added benefits. I feel completely organized for the first time in my adult life. I know where all my stuff is, and I don’t need to go search them out when I need to refer to something. Keeping it current is a snap. And, probably the greatest feeling is the peace of mind knowing that whenever my time is up, my family will have all the information they need at their fingertips.
Knowing that I have done everything I can to ease their burden will allow me to rest in peace.
I believe that being thoughtfully prepared is possibly the greatest gift I can give my family.
It is truly an act of love. |
Why Planning for Death Can Save Your Life
Jon Braddock, July 2018
We have all heard the term “End-of-Life Planning”, but what exactly does that mean? I think for most of us, we think of it primarily as having an Advance Directive. Advance Directive is also referred to as a Living Will or even Medical Directives. These may also include a power of attorney or a health care proxy. Yes, these documents are so important, and everyone should have these in place because these could actually save your life. In short having these documents gives you a voice, when you may not be able to speak!
But for me and from personal experience, I have learned that this is just the tip of the iceberg when it comes to End-of-Life Planning. There is so much more to think about for the day when I am no longer here.
To illustrate what I am referring to I ask this question.
“What do you want the experience to be like for your family and loved ones when you are no longer here?”
Let me share our story of when my wife’s father, Ted, died in 2013. Ted’s death was unexpected, and while our family was dealing with our sudden loss we were doing our best to make funeral and burial arrangements that we hoped would be pleasing to him. We didn’t know what Ted’s final wishes were.
As it turned out, that was only the beginning of our struggles. Soon after the final arrangements were made, and Ted was laid to rest, we began the task of sorting through his finances. Michelle’s father was a private man. He handled all of the household finances and hadn’t really shared any information with his wife or the family.
It took us 10 months of digging through boxes and files and making exhaustive phone calls to locate all of the bank accounts, insurance policies, safe deposits, retirement and pension accounts, online accounts, and more. When we spoke with others about our situation, we found we were not alone. So, while dealing with the normal emotions of sadness and grief, we found ourselves wrapped up in some other not so normal emotions. Those being confusion, frustration, stress and yes, even some anger. These, by the way, are completely avoidable! I’m sure this is NOT what Ted wanted the experience for his family to be like!
Then it really struck me. What if something happened to Michelle and me? Our children are all either still in college or just beyond. They wouldn’t have a clue where to begin or even where to look. Likely, they would never be able to find all of our banking relationships, safe deposit boxes, retirement assets, proof of ownership documents or even our will (as they don’t even know our attorney). Further, how would they access all of our online accounts from social media to auto-drafts and bill-pay accounts. Much less be able to unlock our computers, tablets or smart phones. It would be a nightmare in the highest degree. Frankly, I don’t want to add confusion, frustration and stress after I’m gone.
Let’s face it, life and our stuff, is significantly more complicated than it was 20 or 30 years ago. Technology has made it so. Technology, while simplifying our lives immensely, has made for a very complicated departure. But, it doesn’t have to be that way! We simply need to do some planning. And, it isn’t hard!
Heck, by nature, we are planners. We plan for everything! We make a list to go to the grocery store; we plan what we want to do over the weekend; we plan on what we will wear on that special date; we plan anniversaries; birthday parties; weddings; prepare for births; graduations; vacations; our retirement; we even plan what we are going to have for dinner and what we will watch on TV later tonight. But most of us don’t want to think about or plan for our own death. Why is that?
I think it’s because all those other things I plan for, are for my own benefit. Planning for when I am no longer here doesn’t benefit me, it benefits others. But hey, it is my life and I created this complexity so why should others have to struggle with cleaning it up?
So be thoughtfully prepared. It doesn’t need to be daunting or overwhelming. It is a final act of love and possibly the greatest gift I can give to my family.
I call it Death Etiquette!
In the Next Blog:
I will be discussing the real definition of Death Etiquette, The 10 Things You Need To Know, and simple strategies to get your planning done!
|
The Paradox of Caregiving
Liz Kitchens, July 2018
I’ve been thinking about the role of caregivers. I’ve been reading Orlando Sentinel reporter, Beth Kassab’s honest and thoughtful account of her journey caring for her husband subsequent to his brain cancer diagnosis.l
Likewise, several of my friends have found themselves in the position of caregiving for loved ones. As Baby Boomers hover around the 70 year mark, this role will quite likely become even more prevalent.
A sampling of stories from the caregiving front include:
Suzanne 59, who has been traveling four hours each way to South Florida caring for aging parents who resist the help of outsiders and are unwilling to move into assisted care facilities. Even at home she is in constant communication, all the while trying to maintain her law practice;
The ravages of esophageal cancer has left Jody’s husband disabled and unable to practice law. At 60, she divides her time between her demanding job as a wealth management banker and worrying about her husband’s weight loss and health;
Cathy, 70, is 911 on her adult daughter’s cell phone and has spent up to six of the past 14 months jumping on airplanes to help care for grandchildren. Cathy’s consulting work and board responsibilities have to take a back seat, as does her relationship with friends and other family members.
Kay’s 72 year old husband received a death sentence in the form of a pancreatic cancer diagnosis and died within weeks leaving her and their children reeling.
Nora, 64, is a successful lawyer and mediator in a firm she has shared for years with her husband. Her husband developed a serious liver condition forcing his departure from their firm. She also devotes every weekend during winter months to the extensive health care needs of her aging parents.
Last February I found myself in the role of caregiver (albeit in a much less demanding role than the ones cited above). My charges were on opposite ends of the age spectrum. The first stint was in Chicago caring for grandchildren. At 64, I’m years removed from the ever present needs of little ones- noses to be wiped, naps, snacks, scheduled meal times, potty training, sticker rewards for poops in the potty. The twenty degree Chicago weather and wind limited our outings. It was just too much trouble putting on and taking off mittens, parkas, hats, and boots.
On the heels of this caregiving gig, my husband underwent sinus surgery, the recovery for which was around four weeks. Florence Nightingale I promise you I’m not but I managed to change bandages and ice packs and perform my household jobs and his as well.
Even just changing dirty diapers and bloody bandages I was struck by the intimacy intrinsic in this level of caring. Human beings are full of contradictions. From elementary school onward we spend an inordinate amount of time focused on how we appear to the world. We carefully construct a narrative about ourselves, one usually masking our vulnerabilities. Our motivation in part stems from the fact we are trying to get people to like us, be attracted to us, and to form connections. How can anyone like me if they are allowed to see me without make up, with bed hair, or in a foul mood? So we hide.
True intimacy and connection (which deep down we crave) evolves through vulnerability. We are most vulnerable when we are new to the world and on the precipice of exiting the world. For the caregiver of the young and the older, we are truly needed. Boundaries between people are erased.
Generally, these roles are not invited but thrust upon us. The stories cited above reflect the difficulties involved in caregiving- the time away from our own lives and choices, the exhaustion, the expense, all natural responses to the situation. But juxtaposed to the hard stuff is the good stuff- the love, tenderness, and intimacy. We often dread the prospect of becoming a caregiver. But these experiences offer an opportunity to deepen our connection with our loved ones and recognize in ourselves our capacity for love and kindness.
It had been a long time since a little boy needed me so much (and for that matter even a big one!) Just like the Grinch whose heart grew three times, I think my own heart grew a little too following my time as a caregiver.
|
Creating a Wellness Garden to Bring Joy and Comfort Into the Caregiving Experience
Doug McGinnis
May 2018
I've loved gardening and being outdoors since I was very young. My grandmother always told me I was the only one in the family with a “green thumb” and in fact as soon as I could get my hands in the dirt I was planting flowers around the house. Now, many decades later, I still cherish the experience of watching plants grow.
Though I have several garden areas around my home, there is a special garden room right outside my kitchen window. Every morning as I get ready for another hectic day, I'll look out the window and see this little space with flowering shrubs that attract butterflies, bees and hummingbirds. Birds are singing in the small trees that surround the space. Just spending a few minutes watching this natural scene puts my mind at rest, gives me optimism and brings on comforting memories—a sense of wellness. Later in the early evening, after another stressful day has unfolded, I can go out there and sit and breathe in the fragrance of the blooming plants and let my mind calm down and release worries. It's a special, restorative space that helps me gain perspective in this crazy world. It's a tiny bit of heaven that, in fact, anyone can create.
How many times in our lives when we are needing recuperation have we heard someone say, “Get out and get some fresh air!” This is particularly important for the caregiver. It's a needed space to breathe and restore balance. And those being cared for can also benefit and heal in this kind of garden.
The key to creating your own wellness garden is making it personal endeavor. I like to think of the process as finding your own window to let the outside in, whether you are looking out an actual window or finding a spot outside to sit and observe nature. It could be a balcony with a few pots of flowers and herbs, or a garden room made into your own retreat. When you find that space, consider these factors:
1. The amount of light it receives. Flowering plants often require five or more hours of sunlight to flower profusely. If your spot is shady, there are many beautiful foliage plants that offer color, texture and pleasing shapes, plus shade-loving flowering shrubs like azaleas and camellias.
2. Easy access to water. You need to be able to access a water source nearby. No one wants to be lugging water across a long distance. If that's not possible consider drought-tolerant plants. Succulents offer beautiful shapes and work well in containers. I have a very old aloe in a pot that is blooming now with huge flower spikes dripping with nectar, attracting hummingbirds galore.
3. Make the space as low maintenance as possible. All you really need is a few chairs and a small table. The floor can be mulch or crushed stone or pebbles, or a small paver area if it's in your budget. Mulch also cuts down on weeds, but weeding can be a good thing! There is no better way to get rid of frustrations than by going after weeds with a hoe or getting down on the ground with gloves and tearing out the nasty interlopers--it's great therapy after a difficult day!
Your personal wellness garden can easily spotlight the seasons for year-round interest. In spring, azaleas and spring bulbs help shake off the winter blues. Summer brings numerous choices of flowers, and autumn features mums and changing leaf colors on trees. Even winter highlights interesting bark textures. Don't get too complicated, Pick a pallet of colors that please you.
New, easy-to-use solar lights can spotlight your garden space in the evening, and white flowers such as moon vines and white impatiens and white-foliaged caladiums reflect the moonlight. Evening flowers also attract moths, some of which are uniquely gorgeous.
Fragrance is evocative and probably better at waking memories than any other sensory attribute in the garden. New research on honeybees in Australia shows that fragrance actually imprints on the DNA of insects and without it they have impaired long-term memory! I'm not a fan of strongly-scented plants like night-blooming jasmine or even gardenias. Yet I have a small tree called tea olive that exudes a light, apricot-like fragrance in early evening. I look forward to coming home in winter and spring, when it blooms, and sitting in its presence. In China, pavilions are made for "appreciating tea olive". Don't forget a few potted herbs can bring fragrance and culinary use. Make it easy to reach down and crush a leaf or two.
I have a landscaper colleague who loves to bring his vision-impaired friends to the local nursery to take in the smells and textures of the plants there. These new sensations are just as important as color in brightening a boring, hum-drum day.
Can your wellness garden include edible plants? Of course, and they can be beautiful, too. I've mentioned herbs, but even a small space can incorporate leafy vegetables like mustards, leaf lettuce, bok choi, and chard--and some varieties are super-colorful.
Access is particularly important when growing edibles. Access that serves both you and the one you are caring for. This means you might need raised beds in the growing area. There is no better sense of accomplishment than planting something and watching it grow, nourishing it, picking it, and eating it! And don't forget pulling out those damn weeds!
The more experienced gardener may want to consider water features and bird feeders. My garden is designed to attract pollinators. Watching a hummingbird zoom in and sip nectar while at a nearby flower a monarch butterfly is fluttering about is a breath-taking sight.
Butterflies need both nectar-producing flowers and larval food--plants that attract them to lay eggs where their caterpillar stage can eat. Most larval food plants, such as milkweed, parsley, fennel, etc., tolerate the munching quite well. I have a friend who raises extra tomato plants just so tomato hornworms can eat the leaves and become hummingbird moths! She has hoya vines all around her patio and these huge moths come in the evening to sip nectar from the hoya flowers.
My life has always revolved around honeybees. Most of us have heard by now that honeybees are declining. One of the best things everyone can do to help the bees is to plant flowers. Bees need pollen for their young and nectar for their own sustenance.
I plant flowers with more tubular shapes for the hummingbirds and butterflies, and more "daisy-like" for the bees. Hummingbirds love red flowers, and bees don't see red, but prefer flowers white, yellow, and blue.
My hope is that this very quick overview will inspire others to create small, easy-to-care for wellness gardens. There's a world of helpful tips available online and at your local county extension office. Bringing the ones you care for into the outside world of nature, with sights, smells and sounds is a primal adventure, even if it's from an open window. Letting go of the noise and frustration of the hectic world we create and centering on the quietness and peace of nature is an easy exercise for both the caregiver, and the person cared for.
|
Exercising with an older adult who has limited mobility
A social component to exercise~having shared goals
by Toni Silva Certified Fitness, Yoga, Pilates Instructor with Zero Gravity Fitness
In a workshop that I recently attended, YogaFit® for Caregivers, we discussed the concept of “care partnering.” Quite often, those of us in a caregiver role feel there is no end or stopping point to our days and nights of being a care giver. Often times, it is unlikely that we ask for help, feeling solely responsible to help a loved one – thus forgetting or overlooking our own needs.
Before we can care for others, we must first care for ourselves.
~author unknown.
A new trend I learned about in the YogaFit® for Caregivers workshop is referring to “care giving” as “care partnering.” By making this slight change in perception or labeling, the care provider may feel less alone and responsible for the “care receiver.” In care partnering both people are working together toward a common goal.
With this in mind, fun, playful movement can be equally beneficial for care givers and care receivers. In this blog, I’ve included a breathing and playful workout to try when exercising with an older adult who has limited mobility.
Breathing Exercise
Let’s begin with a breathing exercise to reinforce “care partnering.” Our goal is to empower the older adult with limited mobility to take care of himself/herself and to become an active participant, releasing some responsibility off you.
Start this exercise with your right hand on their left shoulder (they do the same) and possibly seated with knees touching. Explain the exercise first by saying one round out loud, then silently say the affirmation to yourselves but sync breath through touch.
· Breath in and say “care giver” then breath out and say “care receiver”
· Breath in and say “care partners” then breath out and say “care partners”
· Continue this breath exercise for 3-5 rounds. Notice how it feels, centered, balanced, calm, loving, happy. Compassion fatigue is another important point touched upon at the YogaFit® for Caregivers workshop. This is when exhaustion, trauma, and weakness set in due to emotional fatigue from watching a loved one decline, in pain, or dependent. Compassion fatigue can build stress and tension in the body causing chronic health issues such as auto immune, viral infections, or depression.
A way to relieve the body of this stress and help the aging adult with limited mobility is through slow flowing movement. It could be through yoga, dance, sports, tai chi or other technique done with support using a chair or other small equipment. Keeping the movement simple and repetitive is important so care partners can share a common goal to release stress together. Consider including music whenever possible, as music can bring people together through shared experience.
Flowing, Fun, Playful Exercise
Care partners to discuss and plan favorite type of movement (yoga, a simple sport, ballet, etc.) Below is a simple game of catch:
· Choose a favorite music to play for the 5-15 minute session (songs from the care receivers era)
· Next pick 3-5 movements that are relevant (lift, throw, catch, lower)
· Then gather any small equipment needed (soft textured ball)
· Start with 3 repetitions, increase in time and duration as you see appropriate.
These are some simple ideas to try with your care partner. If at first you don’t succeed, you’re probably running about average. It isn’t easy to determine what is going to work, though I encourage you not to give up on care partnering. It can be quite powerful for both of you.
Source: YogaFit® for Caregivers, August 2016, Kelli Braud
DISCLAIMER: This blog offers health and fitness information and is designed for educational purposes only. You should not rely on this information as a substitute for, nor does it replace, professional medical advice, diagnosis, or treatment. You should consult your physician or other health care professional before starting this or any other fitness program to determine if it is right for your needs. Do not start this fitness program if your physician or health care provider advises against it. If you experience faintness, dizziness, pain or shortness of breath at any time while exercising you should stop immediately. The use of any information provided on this site is solely at your own risk.
|
A GAP YEAR FOR GROWN-UPS
by: Liz Kitchens
January 2018
Gap Year: Definition
A gap year is defined as a break between high school and college with the aim of promoting maturity and perhaps the ability to absorb the benefits of higher education. (My personal experience tells me gap year or not, maturity, at least for millennials, does not really happen

until around 30). Well Toto we’re not in high school any longer by a long shot but people facing retirement or semi retirement are increasingly taking gap years to consider a new direction for their lives. For mid career and older workers who have the financial means and job flexibility (a big if) gap experiences can help inform them about what they want to do in retirement. A New York Times article featured Gastroenterologist Dr. Dennis Sinar who took a break from his practice and professorial duties and apprenticed at a stonemasonry in Alaska learning to create stone facings for houses. Thereafter he traveled to Romania to work with a team of archeologists restoring a castle. Dr. Sinar said his retirement has been shaped by his gap experiences.
A hobby writing fiction has blossomed and he has published two collections of short stories. “I never would have thought of making that kind of a stretch before”. And that is the key word- stretch. To introduce yourself to opportunities and avenues you never knew you might enjoy. We have spent so much of our lives in service to an employer, our children, our parents, friends, even volunteer boards, leaving very little time to explore creative ventures that might be self-fulfilling. And not all of these ventures are prohibitively expensive. Sixty-three year old Kathy Thomas says paid or subsidized jobs have kept down the cost of her gap experiences. She has worked at an elephant sanctuary in Thailand, volunteered for six weeks at a home for abused girls in South Africa, attended a weeklong writing retreat in North Carolina, and tended fields at an organic farm in Scotland. She has received room and board at all of these locations, cutting the cost of such adventures exponentially. Worried about early mortality since many family members had not lived past 69, she was eager to try on new experiences while she was able.
Tired of the administrative aspects of doctoring, 74 year old Oncologist John Siebel wanted to retire but treat patients part time. He became a temp covering for vacationing oncologists in locations where he wanted to travel. He is booked for short stints in remote parts of Alaska, California, and Idaho near wilderness areas. Weekdays he sees patients, weekends he explores mountains and wilderness areas.
A growing number of older Americans are experimenting with the concept of a self-designed retirement. Even if we don’t have Dr. Siebel’s skill set, we have our own set of important skills, which can enable us to have work flexibility. So, whatever you want to call it- gap year, semi-retirement, work flexibility, or a self-designed retirement, this is not your Mom and Dad’s version of retirement. Make it your own. Envision a new life going forward. To help in that quest, take this personality quiz designed for the 60+ demographic to assess your own needs, values and motivations at this point in your life. You might just surprise yourself.
|
November 2017 Part 3
When Caregivers Fall Out of Love
How to keep the connections strong when feelings change
by Barry J. Jacobs
“I don’t love my husband the way I used to,” 55-year-old Eleanor, a former client of mine, said sadly. I could understand her sentiments. After her husband had a large brain tumor removed the previous year, his thinking had slowed and his personality became passive. The wryly funny man she’d married three years before was now mostly absent. Should she stay in their marriage even if it had radically changed and she felt burdened by caring for him? She wanted to somehow make it work. “I’m a moral person and respect my vows,” she said. “I’m trying to learn to love him differently.”
With a nationwide divorce rate still hovering around 40 percent (though it has been slowly declining for years), it is hard enough for committed relationships to survive in the long term. But estimates of the divorce rate for couples in which one spouse has a serious chronic illness is as high as 75 percent. Spousal caregivers are said to be more prone to depression than adult children who are caregivers. These spouses often lose not only physical intimacy with their ill loved ones, but also deep friendship if those partners are no longer emotionally or cognitively capable of serving as their confidants. They frequently have to mourn their past joys as a couple along with the dreams they had held for future happiness.
If spousal caregivers like Eleanor decide to stay in their relationships, they often are wracked with resentment because they are giving so much more than they’re getting back. If they decide to leave, they are frequently wracked with guilt for abandoning the people they are supposed to love. While no easy answers exist in these dilemmas, there are strategies for minimizing the deleterious effects of illness and putting the relationship on a new and stronger ground going forward.
Rebalance the relationship as much as possible: Healthy relationships are usually balanced; there’s an almost equal give-and-take between partners. But caregiving relationships, says Northwestern University psychiatrist John Rolland, are necessarily “skewed,” or imbalanced, because the well spouse has to do most of the work. If these relationships become too tilted, then caregivers are at the greatest risk for falling out of sorts and out of love. To whatever degree possible, well and ill spouses should try to minimize these skews and maintain a two-way give-and-take. Ill spouses should continue to try to do whatever they are capable of — simple chores, listening well, giving thanks — for well spouses. Well spouses should refrain from hogging the glory by taking over all responsibilities and disempowering the ill spouses.
Find a different way of loving. According to psychologist Polly Young-Eisendrath in her book The Present Heart, spousal caregivers like Eleanor have to decide whether they can accept a different kind of love — a cherishing of their partner, rather than the head-over-heels passion upon which the relationship originally was based. Such shifts often occur naturally as couples age, but may be greatly hastened by caregiving. Eleanor and other caregivers could admit to themselves that they are staying in their relationships because (to cite several examples) they have a shared history with their partners, retain genuine fondness for them, or feel a moral obligation to be there. It is a different type of connection — perhaps not as fulfilling — but still potentially satisfactory.
Look outside for support you can’t get inside. Most marriages don’t meet each spouse’s every need. That’s why it’s so important to maintain regular contact with friends with whom you have common interests. In instances when an ill spouse can do little to meet a well spouse’s emotional or intellectual needs, good friends become all the more indispensable to supply the care and camaraderie that may no longer be possible within the marriage.
Consider separating caregiving from marriage. Over the years, I have met several ex-spouses who remained committed to caring for ill spouses even though they no longer wanted to be married to them. They lived separately or together in “like,” if not in love, allowing the caregivers to meet moral or emotional imperatives to help — while still being free to seek other relationships for their own benefit. Such arrangements are not for everyone, but underscore an important point for all spousal caregivers: You need not completely sacrifice your own needs to honor vows as a reliable caregiver.
|
November 2017, Part 2
Preserving Your Marriage While Caregiving
Spreading yourself too thin dilutes the attention you can devote not just to anyone in your family, but to everyone in it
by Barry J. Jacobs
My wife, Julie, and I were considering going to the movies on a wintry Sunday afternoon. When I suggested we bring along my frail, 83-year-old mother, Julie didn't exactly say no. But she didn't respond with a "Sure thing!" either. For a variety of reasons, we wound up not going to the movies that day. In all fairness, Julie has been more than a trouper during our years of providing care to my mother.
It was Julie's idea to move Mom from Florida to an apartment within a mile of our Pennsylvania home. That was in 2010, and Julie has made dinner for my mother every Sunday night since then. Like me, she has also taken my mother to countless medical appointments, supermarket runs, concerts, family events and, yes, movies. But there are times when three's a crowd.
Especially since we became empty nesters, Julie and I would like to enjoy some "unchaperoned" time together as a couple. In truth, Mom doesn't expect us to be her social directors; she understands that we have our own busy lives, and she neither pressures us nor complains.
The problem has been mostly me.
I sometimes feel guilty for neglecting my mother when I leave her out of our plans. I also feel guilty for imposing on my wife when I invite my mother to our house or on an outing.
As I've told many a family caregiving client, guilt is a cul-de-sac: It leads nowhere. But finding the right path forward — as a son and as a husband — has been hard. Even when I know I'm doing my best, I guiltily question whether it's good enough.
So in the interest of preserving your marriage while caring for a declining parent, here are some ideas I've found helpful in maintaining mine:
Lower your expectations
Though we all play multiple roles in a family — you may be a spouse, a sibling, a parent, a child and a relative simultaneously — you can never be all things to every family member. Accept that! Even when the care of an aging parent is pressing, it can't become all-consuming without shortchanging your other family bonds. For example, I've had to learn to balance my efforts for my mother with my responsibilities to my wife and children. This means facing up to the fact that spreading myself too thin dilutes the attention I can devote not just to anyone in my family, but to everyone in it.
Performing conscientiously and adequately — even if imperfectly — has had to become good enough for me.
Seek consensus
We all feel entitled to have our needs fairly met, but fairness among family members is a matter of opinion — and sometimes disagreement. I try to talk openly with both my wife and my mother about the constraints on my time and energy. I've tried to establish a running dialogue in which all of us feel heard, and a spirit of negotiation and compromise holds. When Julie and Mom feel I'm taking their needs into account, they're likelier to forgive my shortcomings.
Parents matter — but spouses are paramount
Driving my mother to yet another medical test, taking her to the ER when she's fallen again — isn't it easy to get swept up in the "tyranny of the urgent"? But as important as my mother's well-being is to me, I didn't marry her. My wife is the person with whom I've chosen to spend the rest of my life — presumably long after my mother is gone. That means I must carve out time for Julie and me to enjoy each other's company, but also to solve the everyday problems that arise in the course of our shared lives. So when I find myself "de-escalating" my mother's less-urgent needs to focus on Julie, I try to recall that that's OK: A husband and wife in sync make a better support team for an aging parent.
Say yes to help
Reaching out for help to other relatives and professionals has been crucial for preserving my marriage. For the last two summers, my cousin has invited my mother to stay with her for a week at a time, enabling Julie and me to get away on vacation without leaving my mother home alone.
My brother and his partner visit Mom for a weekend every few months — another welcome respite. Finally, a home health companion takes my mother to appointments when I'm in a time bind. These supports help me persevere as the caregiver I want to be — and as the husband I need to be.
Barry J. Jacobs is a clinical psychologist, family therapist and the author of the book The Emotional Survival Guide for Caregivers: Looking After Yourself and Your Family While Helping an Aging Parent (Guilford, 2006).
|
November 2017 Part 1
In Sickness, Health and (Sometimes) Anguish
Ways to help lower the risks of physical and mental exhaustion for spousal caregivers
by Barry J. Jacobs
The harried 67-year-old wife, though still devoted to her longtime husband, couldn't stop complaining about his selfish behavior. "Ever since he was diagnosed with Parkinson's disease a few years ago, I haven't minded helping him get dressed and walk; I even cut his meat," she said. "But I can't stand how demanding he's become. And he never thanks me."
She is one of millions of American spousal caregivers who have taken their vows of "in sickness and in health" to heart. In the process, she has made many sacrifices to take care of him. She resigned from her part-time job, gave up her walking club and cut back on babysitting their grandchildren. But he seems oblivious to all she's done, constantly fretting about his increasing tremors and the timing of his next pill.
The wife's complaints are reflected in the results of a recent AARP and United Hospital Fund survey of 336 spousal caregivers (part of the larger Home Alone study) that found, compared with caregivers who are the adult children of aging parents, those spouses tend to be older, poorer and more likely to be living in the same household with the care recipient and performing nursing tasks.
They also are more likely to have medical issues of their own, suffer higher rates of stress and receive less external support from family members and friends. Seventy percent felt they had no choice but to provide care.
When I meet with such spousal caregivers in my psychology practice, I observe many of the struggles indicated by the study. Most spouses want to do the right thing for their beloved partners but are ground down by ongoing demands and demoralized by the lack of acknowledgement they receive. They often become more socially isolated over time. They sometimes become depressed.
Here are some ideas that may help lower the risks of physical and mental exhaustion for spousal caregivers.
Compartmentalize being a loving spouse and a dutiful nurse
Caregiving often changes the dynamics between partners — from sharing the joys of living and planning a brighter future to merely surviving the numbing drudgery of daily care tasks. Some of the passion and friendship may go out of the relationship; sadness or even mutual resentment can creep in. To minimize these effects, spousal caregivers should strictly segregate caregiving activities from their own time together as a couple, and thereby try to preserve the kind of interactions that have always been a part of their married life.
For the wife of the husband with Parkinson's disease, that would mean setting aside hours during the day when she and her husband will only be allowed to talk about nonmedical issues — for instance, their grandchildren, holiday plans or the unguarded exchanges of lifelong confidantes. At other designated periods, they would go about the business of toileting or administering pills as quickly and efficiently as possible. Better yet, if the couple can afford it, they could hire an aide to handle the nursing duties so that the wife can concentrate solely on being an emotional partner.
Seek willing and knowing support
Adult children caregivers are sometimes treated as virtual heroes, praised highly for pitching in at all for their aging parents. Spousal caregivers, on the other hand, are frequently taken for granted, as if limitlessly caring for their partners without any concession or complaint was part of the original and binding commitment they'd made. In seeking social and emotional support, therefore, spousal caregivers should be selective, seeking out others who have had similar experiences and who will be more effective supporters.
One possible choice for our wife described above would be to find a local support group through a disease-specific organization such as the National Parkinson Foundation. Another possibility is to contact the Well Spouse Association, a national organization that's made up of spousal caregivers coping with a broad range of medical conditions and that sponsors support groups throughout the United States and Canada, as well as a telephone support group and online message board.
Ask the ill spouse to give, not just receive
Spousal caregiving over time tends to create more imbalanced relationships. The more the caregivers give and the more the ill spouses take, the more likely it is that the latter will increasingly identify themselves as patients who require all the attention. They need to be reminded that (medical conditions permitting) they are not completely incapable of giving back to the partners who care for them — at the very least, expressing heartfelt gratitude. This can go a long way toward bolstering spousal caregiver morale.
The wife should bluntly tell her husband that, even if Parkinson's disease prevents him from washing dishes or mowing the lawn, he can still listen to her feelings and not be so wrapped up in himself. This won't hurt him. To the contrary, it will prompt him to be her partner and more mindful of providing love and comfort as the two of them face life's adversities.
Barry J. Jacobs, a clinical psychologist and family therapist, is a member of the AARP Caregiving Advisory Panel.
|
5 Exercises You Can Do Before Getting Out of Bed
Toni Silva, October 2017 |
As caregivers, we often feel exhausted or stiff getting out of bed in the morning from the intense responsibilities of caring for another person. At times, we might even feel pure exhaustion from not getting a full night’s rest. This is when a little exercise can help.
How we feel physically has a direct influence on our day. Physical activity will generally bring on positive feelings and a more positive outlook. By starting with small movements as soon as we wake up in the morning, we can get our blood flowing, generate warmth, and build energy.
Below are FIVE “go to exercises” that will take your spine through each plane of movement while strengthening supporting muscles. The gentle moves will increase energy, build strength and improve flexibility so we feel less stiff and able to conquer the day ahead. To begin, we must put aside a few extra minutes in the morning. This daily exercise routine can be completed sitting at the edge of the bed in 10 minutes or less.
(Be sure to get your doctor’s approval before beginning any exercise regimen. Use caution, if you have a diagnosed spinal injury).
Start by sitting at the side of your bed with feet touching the floor, bed frame, or place a stool under your feet. It would be beneficial to do 5 sets of each exercise. You may consider increasing repetitions as you begin to feel stronger.
1.Seated Cat/Cow: Hands on thighs with elbows reaching out and away from body. Inhale: lift your chest to the ceiling. Exhale: round your back with chin toward chest and pull navel into your spine rounding your back. Repeat.
 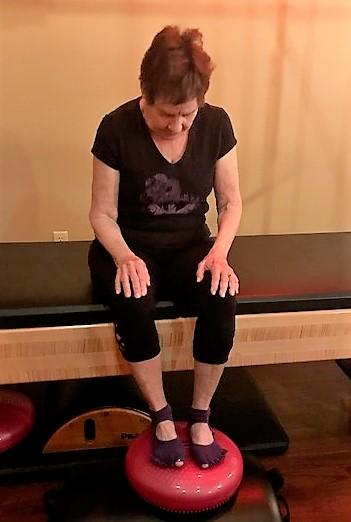
2. Head turns: Sitting upright with hands relaxed on thighs. Inhale: Look straight ahead. Exhale: Turn your head to the left. Inhale: Return to center. Exhale: Turn your head to the right. Inhale: Return to center. Repeat sequence by alternating lead sides each set.
3. Side Bends: Hands on bed beside your hips. Inhale: Lift your right arm Exhale: reach overhead side bending to your left. Inhale: Return right hand above right shoulder Exhale: return right hand next to hip on bed. Repeat on the left to complete one set.
 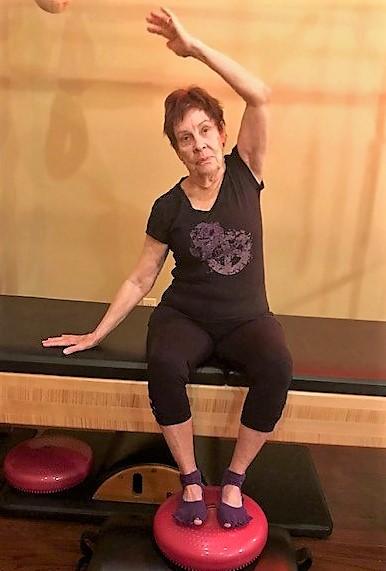
4. Seated Twist: Inhale: lift your arms up to lengthen both sides of your waist, Exhale: rotate your ribs to the right taking your left hand/arm across your right thigh and turning your chest, shoulders and head in the same direction. Stay for a full inhale while lengthening taller and exhale. Return your gaze forward and unwind the body. Repeat twist to left with right hand/arm across your left thigh to complete one set.
 
5. Knee Circles: Inhale: raise your right foot off the floor as you lift your right knee toward your chest with hands on back of thigh or holding onto bed. Imagine you’re drawing 3-5 circles with your knee on the wall in front of you while activating abdominals (pull naval to spine) and lengthening your spine upward. Reverse the knee circles. Place right foot down and repeat knee circles on the left side to complete one set.

Now, feel the changes in your body as you stand up and seize the day!
DISCLAIMER: This blog offers health and fitness information and is designed for educational purposes only. You should not rely on this information as a substitute for, nor does it replace, professional medical advice, diagnosis, or treatment. You should consult your physician or other health care professional before starting this or any other fitness program to determine if it is right for your needs. Do not start this fitness program if your physician or health care provider advises against it. If you experience faintness, dizziness, pain or shortness of breath at any time while exercising you should stop immediately. The use of any information provided on this site is solely at your own risk.
|
| |
"What Japan Can Teach America
About Family Caregiving"
Barry Jacobs, August 2017 |
One after another, three young social work students stood up and tearfully shared their experiences of growing up caring for grandparents with dementia in their family homes. Later, a middle-aged physician talked with pride about frequently visiting his still-healthy, 94-year-old mother to support her choice to live in her own apartment. These were prime examples of “filial piety”—the millennia-old, ingrained tradition of devotion to elders—that I had anticipated.
But there was much I didn’t expect. A social work faculty member ruefully described the growing phenomenon of adult children who had moved to the big city for jobs and no longer wanted responsibility for their aging parents, alone and isolated in their home villages. Such careerists had divorced themselves morally and emotionally from their parents, leaving it up to local government to tend to them.
These were the sharply contrasting attitudes about eldercare that my wife, Julia L. Mayer, Psy.D., and I heard during a recent visit to Japan. We had been invited to give lectures on aging and resilience at the Kanagawa and Tokyo campuses of Tokai University as part of a year-long celebration to mark the founding of the university’s Faculty of Health Management, an ambitious, interprofessional program of professors, researchers and clinicians from a broad array of medical and social sciences. The divergent sentiments we heard at our lectures offered lessons—and perhaps a glimpse into the future—for America’ aging families and caregivers.
This was my first trip back to Japan since I spent a college semester there in 1979 to study its Confucian culture. I found much that was still familiar to me, including the country’s sometimes jolting blend of old traditions—such as its love of tatami mats and hot springs baths—with the ultra-modern—such as uncannily efficient subways, ever-present vending machines and green tea Kit Kat bars. But the Japan I knew from nearly 40 years ago has gone through an extreme demographic shift because of increasing life expectancies (now 4 years longer than in the U.S.) and decades of low birth rates. (There are supposedly more pets than children in Japan today and more diapers sold for adults than babies.) It is now far and away the most rapidly aging nation in the world with about the same population as when I was last there (120 million) but triple the proportion of people over 65—over a quarter of the population. That number is expected to rise to an astounding 40% by 2060. U.S. senior citizens, in contrast, now comprise 15% of our population and will top out at only 20% in 2030.
Japan has been whipsawed by its demography and is consequently experiencing contradictions and ambivalence about eldercare. In the 1990s, many Japanese women were overwhelmed with caregiving and work duties; reports of caregiver abuse of older relatives began to rise. The government responded in 2000 with a mandatory long-term care insurance program for all Japanese over age 40, as well as the introduction of such community-based services as case management, adult day care centers, and home companions. Today, the tradition of “sansedai kazoku” (three-generation households) still exists among 60% of the populace. But, according to a 2014 Pew Research Center survey, 87% of Japanese think aging is a “major problem” for the country (the world’s highest percentage) and only a third of them believe that families should bear the “greatest responsibility for the elderly.” (Thirty-six percent think it’s the government’s job.) There have been more and more highly publicized cases in which family caregivers murder the parents they’re caring for and then commit suicide. Filial piety, it seems, is on the wane.
What can Americans learn from Japan’s struggles? Here are two thoughts:
When the number of aging citizens reaches certain thresholds, societies must respond with increased services: If there was any country whose long tradition of family values would have sustained its commitment to eldercare, in my mind, it was Japan. But the sheer volume and needs of the old began to crush even stalwart Japanese. Its government responded accordingly and appropriately. When America’s aging “problem” increases in the next 15 years, will our local, state and federal governments respond with the same compassion and thoughtfulness? I hope so but am concerned. As with Japanese society, there will be dire consequences for U.S. individuals and families if we don’t devise and pay for the right supports.
When governmental supports are put in place, family commitments change: Because of Japan’s long-term care system, including increasing numbers of residential facilities, more Japanese feel entitled to have the government support their aging parents. That is a radical departure from Confucian tradition. Could the same happen in the U.S. if our long-term system was greatly expanded? Would Americans have less compunction about walking away from a perceived caregiving “burden” if they knew that the safety net for their parents was actually safe and strong? I don’t know the answer but expect that, as our caregiving systems necessarily change in the next two decades, our family values will, too.
Barry J. Jacobs, Psy.D. is a clinical psychologist, family therapist and the Director of Behavioral Sciences for the Crozer-Keystone Family Medicine Residency Program in Springfield, PA. He is the co-author (with his wife, Julia L. Mayer, Psy.D.) of AARP Meditations for Caregivers—Practical, Emotional and Spiritual Support for You and Your Family (Da Capo)
|
 |
Meet the CCI Ambassadors
Liz Kitchens, May 2017 |
My passion is to build a community of support for caregivers but not
In a way that is most obvious. Certainly supporting caregivers and their care partners with their physical needs is critical. What my family foundation, The Pabst Foundation, seeks to nurture is emotional support for caregivers and their families. We support The National Center for Creative Aging's program, The Creative Caregiving Guide to do just that-- emotional and social support for caregivers.
I am proud that Diana Silvey from The Winter Park Health Foundation is a key ambassador in this effort. Thank you Diana for all you and the WPHF do in our community!
~Margie
May 2017:
Meet the CCI Ambassadors: Diane Silvey, Winter Park Health Foundation
I recently met with Diana Silvey, Program Director at the Winter Park Health Foundation. Full disclosure, Diana is a dear friend, and someone passionate about health issues facing older adults and their families. Diana moved to Florida ten years ago to work at the Foundation in part because she valued their mission statement: to make a positive difference in people’s lives by creating the healthiest community in the U.S.
Diana also values place-making, which is creating public spaces that promote people’s health, happiness and wellbeing. She gave me a virtual tour of what will be The Center for Health and Wellbeing due to open in Winter Park, Florida in late 2018. This public space, inspired by nature, will feature gardens and social gathering areas. This center is the result of collaboration between the Winter Park Health Foundation and Florida Hospital, and will offer medical offices, physical therapy and rehab services, a healthy café, teaching kitchen, and an interactive resource space dubbed the Healthy Living Experience. The Center will also be the new home of the Peggy & Philip B. Crosby Wellness Center YMCA, with plans for it to become a medically integrated fitness facility.
But those are just the overall details of this place. Let me try to describe the vision of this space as explained by the architect, Turan Duda. A common theme of the center is the number 7. There are seven gardens ranging from a meditation grove, providing a corner for meditation and reflection to beds of edible herbs and vegetables.
Keeping with the theme of 7, the project focuses upon the Seven Dimensions of Wellness. These dimensions include:
* Intellectual wellness, being open to new ideas, creative thinking, learning and seeking out new challenges
* Physical wellness, caring for the body for optimum health and functioning
* Social wellness, building relationships with a positive social network
* Spiritual wellness, finding meaning and purpose
* Vocational wellness, seeking a career or other work that is interesting and fulfilling
* Emotional wellness, having a positive attitude, self-esteem, sharing a broad range of emotions with others in a positive manner
* Environmental wellness, awareness of interaction with the environment and the community
Seven is the number of completeness and perfection (both physical and spiritual).
The number seven is prevalent in nature -- we have seven continents, seven oceans, the rainbow has seven colors, there is even Seven Wonders of the World. Not only is the number seven important to this design concept, so is the Golden Ratio.
As a clay artist, I have read about the golden ratio as it relates to nature and design. Turan Duda has employed the Golden ratio (an age-old mathematical concept) in his design of the Center for Health and Wellbeing. There are countless references in nature (the leaves on a tree and the spiral of the seashell) and art – The Parthenon, Mona Lisa, and the Last Supper. When followed, the effect is peaceful and calm, subliminally pleasing to the viewer/listener.
With more and more individuals seeking ways to age with vitality, this Center will be the first in the nation offering wellness, fitness, and medical care all under one roof, potentially changing lives and enhancing wellbeing. This space is the epitome of place-making- creating public spaces that promote people’s health, happiness and wellbeing. I, for one, can’t wait for the opportunity to enjoy this space.
|
 |
"Angry Caregivers’ Misguided Blame"
Barry Jacobs, April 2017 |
“What made you decide to end your marriage?” I asked the exasperated 42-year-old woman in my office.
We were having one of those post-op individual psychotherapy sessions shortly after the couples therapy I conducted with her and her husband had failed. Our bid to save her marriage had gone poorly from the start. A year ago, her husband had had a major heart attack that killed 40% of his heart muscle and left him weak and highly anxious. Every time he felt chest pain in the months afterwards, he was convinced he was having another heart attack and repeatedly called 911 to carry him out of his workplace on a stretcher. (No further heart damage was ever detected in the emergency room.) As a consequence of these disruptions, several different employers had fired him in quick succession. During our couples sessions, he pleaded with his wife to be patient with him until he found a position that suited his now diminished physical abilities and he regained confidence in his health and safety. But she eyed him coldly and expressed no empathy—only anger.
“I’m tired of working and working and working,” she complained to me during our individual meeting. “I have to take care of the house and do hair and everything. And he just doesn’t do anything. I’m tired of him saying he can’t do things.”
“But don’t you think his heart condition has changed what he can do?” I responded.
She shot back with rising irritation, “No. It’s all mental. He’s never been able to keep a job. Not since the beginning of our marriage 17 years ago. And he’s just trying to use his heart now to manipulate me to take care of him. But I won’t let him do that anymore.”
Her view of him was as unshakeable as it was unforgiving. They separated soon after. She wound up starting her own small business and eventually marrying an older, affluent man who catered to her. He crashed on friends’ couches for a few weeks before moving into a homeless shelter. He only got back on his feet when he found another woman to take him in.
So what’s wrong with this picture? He was a lousy provider, in all likelihood, who’d made her feel victimized for nearly 17 years. She had every right to decline being re-victimized as his put-upon cardiac caregiver. Some would call that karmic justice.
But what happened here, in my mind, wasn’t simply an illustration of a bad relationship history undermining the willingness to make sacrifices on another’s behalf. She attributed malice to her husband’s intentions. At the same time, she trivialized his disabling heart functioning and resultant anxiety. It was as if she believed he was a malingerer and sociopath who willfully interpreted his chest pains as heart attack symptoms just to ride the ambulance and get out of a day’s work. To me, this was a distortion of the medical reality. Worse, it was a kind of character assassination that amounted to kicking a man when he was already down.
This happens in family caregiving in more subtle ways all of the time. Think of the emotionally distant adult daughter who avoids dealing with her father with dementia because he had always been mean to her when she was growing up. She perceives his yelling now as more of his old orneriness and not the agitated protests of a diseased mind. Or consider the wife of a lung cancer patient who blames him for ruining his life and hers because of his heavy smoking. Not every one of these family members will sever their ties with the care receiver when the time for caregiving arrives. Some will keep their distance and give little. Others will give lots but do it with an edge of resentment while assuming a bossy, morally superior stance.
This kind of blaming may feel right. But I think it’s misguided. Ill-used caregivers are entitled to walk away but do themselves no honor assuaging their guilt through being vindictive toward the newly vulnerable. That turns caregiving into a grudge match which compounds the suffering of the already disabled care receiver. It precludes any possible joy in the caregiving. It impedes real understanding of and empathy for the present predicament. We need to carefully distinguish the clinical symptoms of aging and illness from the past’s negative emotional legacy or risk conflating the two. Heart attacks needn’t prompt attacks on the heart.
|
 |
"The Arts As A Beacon of Hope"
Liz Kitchens, March 2017 |
I’m a big fan of the National Center for Creative Aging (NCCA). Their mission statement says they are dedicated to fostering an understanding of the vital relationship between creative expression and healthy aging. Anyone who has engaged in even a cursory read of the Be Brave. Lose the Beige blog knows I’m a huge proponent of creative expression. Studies have demonstrated participation in the arts promotes physical and mental health, particularly among aging adults.
I was fortunate enough to attend the launch of the Creative Caregiving Initiative at the Arts and Wellness Symposium last fall in Orlando. The NCCA has developed an online caregiver toolkit. The toolkit contains artistic exercises for caregivers and their loved ones. Part of the focus is respite for the caregiver. This was the brain-child of Margie Pabst, of the Pabst Foundation for the Arts. She says, “The life of a caregiver is often filled with isolation, loneliness, stress and depression with patches of sunlight and hope. We saw the arts as a beacon of hope.”
While this initiative is targeted primarily to caregivers of family members with Alzheimer’s and other cognitive disorders, I see its application for caregivers of all shapes and forms.
As Baby Boomer women, it feels like we have been caring for others our whole lives. We are truly the “tweener” generation, sandwiched between parenting our adult children and tending to aging parents. I know my mother cared for me and loved me but I’m not sure she took hoisted my emotional traumas on to her shoulders in the same way we do with our children. Or perhaps, we just did not share them in the same way we have encouraged our children to share theirs. We looked them in the eyes all those years ago and said things like, “you can tell me anything. “. In many instances we would have gladly assumed their cares rather than witnessing their struggles.
My daughter recently underwent a very real trauma. While intellectually I know the experience was more difficult for her, I don’t know if it could have been that much greater considering the extent to which I felt her pain. Living in another state made access more difficult so there were many telephone calls, plane trips, Face-time sessions, and any other means of communication.
Creativity was an integral part of our care exchange. A shopping cart at Michaels Craft Store was loaded with clay, buttons, paint, and canvasses.
An entire day was devoted to creating. It really did not matter what, it was the process of creating. Hallmark holiday movies accompanied our sculpting and scrapbooking.
My family room assumed an art studio with bits of paper, Fimo clay, and glitter strewn about. So what! Cleaning only took minutes. The process and products will last in our hearts forever.
|
 |
"Pain and Acceptance at the End
of Caregivers' Hopes
"
Barry Jacobs, March 2017 |
“You are treating her like she’s a piece of meat,” Tony was shouting angrily at me. I hadn’t the power to change the care his 62-year-old wife was receiving in my hospital’s intensive care unit—for the past two years, I had been their psychologist, not nephrologist—but, for the moment, I became the embodiment of all Medical Authority. “She just lies there, unconscious and horribly swollen. You don’t do anything for her except stick her with more needles.” The look on his face then shifted slightly from accusatory to imploring. But I couldn’t save her.
His wife, Elena, had been bedbound in their tiny apartment in suburban Philadelphia for at least five years because of chronic, severe back and knee pain. She’d become confined there as the result of a series of personal and medical missteps—or, put another way, lack of steps. Once she’d entered middle age and her girth thickened, her joints had started aching because of the increased weight they supported and she consequently walked less. As she’d walked less and took to her “sick” bed more often, she burned fewer calories but never adjusted her diet and consequently gained more and more weight. Taking handfuls of pain pills every day didn’t relieve her joints and propel her off the mattress; instead, they only sedated her into a supine stupor in front of the TV. And the long-term narcotic use gradually took its toll: Her kidneys and other organ systems were now shutting down.
Tony was her devoted enabler. He’d waited on her slavishly, bringing her favorite foods, sitting bedside with her every day for hours to watch TV and listen to her steady complaints. He owed her, he felt, because she had stuck with him through his wild drinking years until he finally sobered up. He’d paid her back by sticking with her through her retreat from the world and now he was still sticking with her in the hospital, like he thought he was supposed to do. He would plead with the doctors to make her whole. He would utter lengthy beseeching prayers during sleepless nights in the armchair in Elena’s ICU room. But he could see that none of it was working. He was frightened for her life. He was afraid he was letting her down.
My job, it seemed to me, was not to try to persuade her medical specialists to make hail-Mary efforts for Tony’s sake. Neither dialysis nor multiple meds were working. My job was to convince him that Elena’s condition had taken a discernible turn. Family psychiatrist John Rolland of the Chicago Center for Family Health has written compellingly about the phases of illness—acute, chronic, terminal—and how hard it is for patients and families to switch their expectations and actions from one phase to another. We all believe at first that our ailments have a cure until some professional tells us that our condition is chronic and that we will have to learn to live with managing the symptoms. We are all lulled into believing that life with that chronic condition will go on and on until the end hits us shockingly like a sucker punch. This is the hard stop on hope.
“Tony, I’m worried that Elena won’t make it,” I said quietly. He stiffened and said, “No,” but the word sounded more resigned than forceful as if he knew that protesting wouldn’t change anything. We’d worked together for two years and he trusted me. By stating the inevitable first, I was giving him permission to begin thinking about the possibility of her death without feeling guilty. “You’ve been a very good husband to her for a long time,” I went on. And then to suggest a way he could continue to be good to her, I said, “I think it’s time to talk with her doctors about considering hospice.”
“Yeah, well, we’ll see,” he said gruffly. Over the next few days he continued to push her physicians to try new interventions as if defying what I’d said. But our short exchange had a started a process. He didn’t want to accept that she was in the terminal phase but he now knew it. When the doctors themselves approached him with the suggestion of taking her off of life supports, he acquiesced. She died a day later.
In our initial meetings in the months afterwards, he was still angry at her doctors and at what he saw as an uncaring world. But time passed and anger abated and he began to allow himself to feel relieved of the burden of caring for her without also feeling guilt for getting rid of her. “You were a good husband,” I kept telling him. With time, he came to see that that didn’t mean preserving her life, but accompanying her through its vicissitudes, termination included.
|
 |
"Engaging during the Dementia Journey
One Story and Six Tips"
Deborah Shouse, March 2017 |
My satchel was packed with potential connectors, not the electrical type, but the emotional, engaging type. I had a sheaf of favorite poems, an Audubon bird book, a list of songs Mom and I liked, some bright red Mardi Gras beads, several colorful scarves, and some paper and markers. I was eager to see what Mom might fancy and I felt prepared for any creative impulse. But as usual, my mom surprised me. When I walked into her room in the memory care community, she was sitting on the bed, fiddling around with a blanket. She smiled and held out her hands. I sat beside her, held her hands, and smiled at her. She laughed. I laughed. She made a little funny face. I mirrored her. I followed her lead until she suddenly gripped my fingers and closed her eyes. I closed mine, but kept sneaking peeks at her. She was asleep, a lazy smile on her face, so I closed my eyes and rested with her.
Spontaneity and surrender were two of the many lessons my mom taught me during her dementia journey. I loved preparing for our time together, cobbling together ideas to engage us both. Sometimes we sat quietly, leafing through magazines. Other times, I sang Mom show tunes. Still other times, I simply went with the flow and enjoyed Mom’s energy and spontaneity.
My mom has since passed away but her spiritual and emotional gifts linger on. When I visit friends who are living with dementia, here are a few ideas for connecting.
• Choose a quiet space relatively free of distractions.
• Select a time of day when you both have lively energy.
• Bring a project (or projects) you’d both enjoy.
• If the person is shy about creative projects, issue a low-key invitation, such as, “Want to help me with this project?”
• Allow the activity to unfold at its own pace, offering support as necessary and
encouragement along the way.
Enjoy the process.
• If the activity doesn’t go as planned, don’t worry. Go with the flow and relish your time together.
Deborah Shouse is a writer, speaker, editor, former family caregiver, and dementia advocate. Deborah’s latest book, Connecting in the Land of Dementia: Creative Activities to Explore Together, features dozens of experts in the field of creativity and dementia. These innovators share ideas that engage the creative spirit so you can continue to experience meaningful moments of connecting. Deborah and her partner Ron Zoglin raised more than $80,000 for dementia programs by donating all proceeds from her initially self-published book, Love in the Land of Dementia: Finding Hope in the Caregiver’s Journey, to dementia based non-profits. Central Recovery Press has since published an updated version of Love in the Land. To learn more, about Deborah and her work, visit DementiaJourney.org |
 |
"Keeping Connected Throughout
the Dementia Journey"
Deborah Shouse, February 2017 |
As my mom’s dementia deepened, I wondered how I could stay connected with her. Mom and I had enjoyed discussing family issues and books, going to movies, and watching birds. But with her increasing memory loss and restlessness, I realized we would have to forge a new relationship.
Research shows that the part of the brain involved with creativity and imagination outlasts the rational part of the brain, so there are limitless opportunities for engagement. Our new relationship was built of activities such as singing, leafing through magazines, touching flowers, listening to music, cooking together, and laughing.
The benefits of doing creative activities together include more energy and socialization, reduced anxiety, and chances to express yourselves in new and meaningful ways. Increasingly, studies show that painting, drawing, and other arts and crafts reduce the risk of cognitive impairment. Additional activities such as music, movement, gardening, and social interactions strengthen the body, brain, and spirit.
Here are some easy ideas to increase creativity while staying connected and having fun.
Tune into Singing
Singing was one of the ways I stayed engaged with mom during her journey. I always felt happy after singing together. Now a study from Dr. Teppo Sarkamo in Helsinki, Finland, explains why. Dr. Sarkamo’s research found that “regular musical activities can have an important role in maintaining cognitive ability — enhancing mood and quality of life for people living with dementia. These activities also promote the well being of care partners and offer a beneficial leisure activity for both partners.” Dr. Jytte Lokvig, from Santa Fe, NM, facilitates sing along groups in memory care communities. She believes that music is a doorway to creating connections. “Even when I do an art activity, I start with a few songs to knit us together,” she says. Bringing singing into your daily life is a simple way to connect with yourself and with the person you’re caring for.
Cook up a Connection
Cooking is another wonderful way to connect and create together. As her husband Charlie moved deeper into dementia, Elizabeth Miller bought a cookbook from his teenage years, the 1960s. They read through the recipes and highlighted the ones Charlie remembered his mom making. Then, with Charlie as her sous chef, Elizabeth made dishes such as chicken cacciatore, tuna casserole, and spaghetti and meatballs. They invited Charlie’s childhood friends over for a meal and talked about old times
while they chowed down on Johnny Marzetti Casserole.
Working together in the kitchen offers a low-stress way to accomplish a task and relive family and food memories. People want to be useful and creating meals for and with someone meets that need.
Here are some tips:
• Use the foods, the preparation, or the occasion as a catalyst for conversation. Encourage stories and ask open-ended questions.
• Look for seasonal recipes or foods that have delicious aromas, interesting textures or that evoke good memories. Some examples include baking holiday cookies, preparing cinnamon rolls, mashing potatoes, or cranking ice cream.
• Even if the person living with dementia can’t help prepare the meal, he can still enjoy sitting in on the action and the conversation. Having the experience is more satisfying than sharing any dish of food.
Nurture with Nature
“People with dementia often feel a sense of calm and connectedness when they’re outdoors,” says Claire Craig, PhD, co-author of Creativity and Communication in Persons with Dementia: A Practical Guide. “When people are not grounded in their natural surroundings, they can feel disoriented and confused.” Claire sees the outdoors as a place to unite art and nature. Many people relate to the seasons through gardening, farming, and lawn care. Many relish walking or sitting outside, feeling the fresh air, seeing majestic oaks or fragrant pines, breathing in just bloomed lilacs and crimson roses, watching squirrels and hearing lyrical birdsong. “Look at your outdoor space as an opportunity,” Claire advises. “Ask yourself, ‘How can we make this space our own?’ Think of projects you can do as a team. Consider building something simple out of wood. Glue it together if you don’t want to use nails. Decorate planters with paints or paste on shells, tiles, pebbles, mosaic pieces, and more.” Poetry rocks, literally. Claire guides people in gluing short poems, inspirational sayings, or copies of favorite photos onto smooth rocks, then varnishing them. They will fade with the weather but make lovely gifts or garden accents. She also suggests painting rocks. To create a spontaneous outdoor art gallery she pins copies of photos on a clothesline and discusses them as they flap in the breeze.
Weave Activities into your Daily Routine
A good activity should be easy, mutually pleasurable, appropriate for ability, age, and gender, imbued with some meaning, and have no deadline and no pressure. Simply incorporate them into your daily routine and you’ll enrich your time together.
Deborah Shouse is a writer, speaker, editor, former family caregiver, and dementia advocate. Deborah’s latest book, Connecting in the Land of Dementia: Creative Activities to Explore Together, features dozens of experts in the field of creativity and dementia. These innovators share ideas that engage the creative spirit so you can continue to experience meaningful moments of connecting. To learn more, about Deborah and her work, visit DementiaJourney.org
|
 |
"Creative Living Is a Path for the Brave"
Liz Kitchens, February 2017 |
I took my creativity crusade on the road a couple of weeks ago. I was invited to conduct two workshops at The Myositis Association’s annual conference in New Orleans. Myositis takes many forms- Lupus, RA, and severe muscle weakness, to name a few. Art As A Beacon of Hope, the first session I conducted, was designed for patients with autoimmune disorders. Caregivers Living In Color addressed issues facing caregivers of loved ones suffering from these debilitating diseases.
Even though I do not suffer from an autoimmune disorder I wanted to convey my passionate belief that having an illness or caring for someone who does, does not have to doom one to a poor quality of life. Creativity is obviously not a panacea, but it is helpful. A Dose of Creativity, documents the benefits of creative engagement among aging adults- fewer doctors’ visits, the need for less medication, memory enhancement, fewer falls, a sense of belonging, “a second chance at life” according to one of the budding artists in the documentary.
Laura Holson, in a New York Times article entitled “We’re All Artists Now”, wrote:
“Our best selves are merely one doodle away. Where once drawing and other painterly pursuits were the province of starving artists or simply child’s play, unlocking one’s creativity has become the latest mantra of personal growth, career success,
and healing”.
This article talked about how creativity has the same holistic benefits as a weekend at the Canyon Ranch Resort and Spa (and much cheaper, I might add). The Mayo Clinic recommends the health benefits of painting and ceramics. A four-year study found that people who took up creative endeavors at middle age suffered less memory loss.
I came to the conference loaded with statistics and suggestions for creative coping techniques. As is often the case, though, I was the one walking away feeling enriched. I carried home stories about acute pain, muscle inflammation and weakness, negative reactions to medications, falls, even death. I listened to the stories of spouses describing their multiple roles and responsibilities and having little to no time left over for their own pursuits. A young husband became emotional describing how he missed physical intimacy with his wife of only two years. The “toys” people have bought to help them function- motorized wheel chairs, bidets, vans with special lifts. But what I was most moved by was the obvious love and devotion between patient and caregiver. I heard a sweet story from one husband who said his own creativity had actually increased since the onset of his wife’s illness. He cuts out fabric for her as she is no longer able to squeeze a pair of scissors. They have become closer than even before her illness due to these shared activities.
I was struck by the bravery. The fact these attendees showed up to the conference was brave. They aren’t settling for a diminished life. As the name indicates, Be Brave. Lose the Beige advocates bravery. Not necessarily the kind of bravery required to climb a mountain or parachute from a plane. It’s the little every day heroics, like choosing to own your own life rather than allowing circumstances or others to own you.
Elizabeth Gilbert, of Eat Pray Love fame, has written a new book entitled Big Magic, Creative Living Beyond Fear. Gilbert referenced a poet professor who said the following to his budding writer student:
“Do you have the courage? The courage to bring forth this creative work? The treasures that are inside you are hoping
you will say yes!”
Elizabeth Gilbert goes on to write:
“The hunt to uncover these treasures- that’s creative living. The courage to go on the hunt in the first place- that is what separates a mundane existence from an enchanted one. A creative life is a bigger life, an amplified life, one that is more interesting. Creative living is a path for the brave.”
I was honored and happy for the opportunity to meet real heroes this weekend.
You can visit Li’z blog here: http://bebravelosethebeige.com/2016/09/19/creative-living-path-brave/
|
"They Put Me In Places"
Barry Jacobs, January 2017
“They take me—take me and put me in places,” my 86-year-old mother says again. She stammers as if unsure how to describe her baffling experience. Her deeply lined face has a look of discomfort and dread. “Various towns and facilities,” she says haltingly. Then, after a pause, “A shtetl. A kind of shtetl.”
The “they” she is referring to are the nursing home personnel whom she doesn’t particularly trust, even after a year of residing here. She often bridles at their directions and suggestions. Perhaps she specifically means the certified nurses’ assistants about whom she constantly complains for their rough and infantilizing treatment.
Her reference to “shtetl”—a Yiddish term for the small Jewish towns of pre-Holocaust Eastern Europe—is more interesting to me. Her parents came from such a place on the Bug River in eastern Poland and raised my mother and her two siblings in a 6-story walk-up in a poor, heavily Jewish neighborhood in the south central Bronx in the ‘30s and ‘40s. My mother then moved over her lifetime to a succession of Jewish “shtetls” in Queens, Long Island and South Florida before landing in this Jewish nursing home outside of Philadelphia near my home. In my opinion, she has never left the shtetl and now never will.
As a clinical psychologist specializing in geriatrics and family caregiving, I know how one is supposed to respond to a loved one’s confusion due to dementia—with calm, good cheer, and tolerance. As I’ve pointed out to many of my family caregiver clients, becoming upset and trying to correct some bizarre or paranoid idea rarely creates cogency. Instead, it tends to provoke more agitation and therefore more confusion.
But the son in me, bothered by my mother’s bewilderment, can’t simply humor her. “You’ve been here the whole time,” I tell her. “They would have to tell me if they were moving you somewhere.” My mother just looks at me blankly. “If they took you somewhere,” I ask her, “then how did you get back here?”
“I don’t know,” she at first responds. But then she adds, “I took a bus.” I look at her slumped in her wheelchair, knowing she hasn’t been on public transportation for years. It’s folly, though, for me to think that I can re-orient her with mere facts or logic.
Later on, when we call my brother on my cell phone so that she can speak with him, she repeats the story of being moved to various places. I can hear him trying to re-orient her by asking her why they would keep moving her. She responds by saying, “Different strokes for different folks,” one of the cliché phrases she now sometimes uses that have no meaning in and of themselves but which she repeats as a face-saving measure for not knowing what to answer.
There is no end to the confusion. She tells me sometimes about seeing people who have been long dead. She asks me if her parents are still alive. “Of course not,” I say too brusquely. “Really?” she asks, astonished. I shouldn’t be taken aback by her astonishment—it’s the nature of the disease—but I always am.
On the car ride home, I muse about the hour spent trying to sort out what is going on in her muddled head. Could there be some meaning behind her delusions? To be moved without her consent from place to place, as she believes, is to feel a constant state of dislocation and vulnerability that well captures the lost-ness of advancing dementia. There is uncertainty and fear, helplessness and hopelessness, and an awareness of being unmoored.
To believe you are being moved to shtetls conjures other associations for me—and not the ebullience of Tevye in “Fiddler on the Roof.” My mother may have lived in increasingly Americanized versions of Eastern European villages her whole life but she always wanted to escape the ignorance and impoverishment of her parents’ past. There is no leaving that shtetl now (not even by bus). There is no avoiding that sense of being at a cultural and spiritual dead-end. No more middle-class striving. No more embrace of high aesthetics and world travel. No more fancy dresses and sparkly jewelry. Her experiences of today are conflated with memories of her mother’s modest house dress, her father’s aching hands from his work as a window washer.
I’m not sure how to help my mother now. She drifts in her mind to strange and familiar places. I follow, providing what little company, comfort and direction I can.
|
7 New Year’s Resolutions for Hopeful Family Caregivers
The six-and-a-half years that I’ve been caring for my aging mother would seem like a blur of appointments, pills, and thrown-together meals if not for periodic times to reflect. The new year is one such vantage-point. How am I doing? I ask myself. How are we doing? I ask her. What gumption, luck, and juggling are needed to manage the emotional, medical, and financial challenges in the months ahead?
The year is best approached by all family caregivers with hope, the anticipation of positive gratification, and firm resolve. That takes specific resolutions and goals. Here are some of mine for 2017:
I will strive to see the forest for the trees: There is so much to do as a caregiver each day that it is easy to get caught up in the tasks at hand and lose sight of the greater mission. But caregiving is not about checking off chores on an endless to-do list; it’s about making personal sacrifices on behalf of someone you love. When I’m preoccupied with getting through to my mother’s doctors or directing her aides or filling out forms, then I feel mostly frustrated. In the coming year, I hope to keep focused on the positive reason I’m doing what I do—to help my mom live as well as she can.
I will aim for joy, not bitterness: Over the years, I’ve been irked at times by critical family members and aggravated by professionals who don’t listen well and give impractical advice. But I keep reminding myself it’s the small moments that are sustaining. If I can get my mother interested in looking at old photos and sharing family history with me, then that’s a victory. When she smiles, I smile and the day has some sweetness.
I will learn to better compartmentalize: This seems to me the key to emotional wellness—to be present where we are at any given moment. I don’t want to be awake thinking about what happened at my mother’s doctor’s appointment or worrying about work when I’m with her or ruminating about Mom when I’m with my wife and kids. I have to develop thicker walls between the different parts of my life. I have to learn to fully inhabit each room when I’m there.
I will connect with those who are responsive: A truism of family caregiving is that some of the people who we expect to help us don’t, while others who we don’t expect to step up do. Rather than being disappointed with those who failed us, it is better to focus on those who supported us. I should strengthen my connections with those relatives, neighbors, work colleagues, and fellow caregivers who have cared, commiserated, and pitched in.
I will make my requests for help more specific and concrete: Another truism is that “Not all help is helpful.” Lots of well-meaning people tell caregivers, “Let me know if I can ever be of help.” But those undefined offers of assistance generally amount to nothing. People are much more likely to give help if the ask is as tangible—and do-able—as possible. In 2017, I plan to reach out to others with very specific requests for discrete tasks within given time-frames.
I will practice self-kindness: I have great expertise at finding fault with my own caregiving. It’s being kind to myself—appreciating that I’m doing the best that I can, however imperfect it often is—that is the bigger challenge. Beating myself up degrades my morale but rarely leads to improvements in my performance. I want to see myself positively for who I am—a son who tries.
I will be open to transformation: My mother is gradually becoming more limited in her abilities to think and express herself clearly. She is now mostly wheelchair-bound. These changes mean change for me, too, and not just in taking on more tasks. To really be with her, I have to be more patient and compassionate. When she is afraid, I have to reassure. This is growth that can only make me a better and more caring person.
More challenges are coming in the next year. I can’t say I’m ready for all of them.
But I’m willing to adapt, muddle forward, and learn.
|
How to Maintain & Find Happiness While a Caregiver
Research from multiple areas like psychology, medicine, and immunology, have shown that caregiving can be extremely stressful - so stressful in fact that our physical and mental health can be impacted negatively. However, keeping a healthy balance for caregivers is possible with the help of a few tools to manage the stress. The field of positive psychology has investigated techniques and published the research that can help caregivers experience peace and happiness amid the challenging task of taking care of a loved one.
Chronic stress takes a toll on the body by activating the production of various internal chemicals that can end up causing parts of our body to work less efficiently, in particular our immune system, digestive function, and our ability to think clearly. This is due to the chronic activation of part of our peripheral nervous system that controls the “fight or flight” reaction known as the sympathetic nervous system. Its counterpart, the parasympathetic nervous system, calms everything down and is known as “rest and digest”. Every day these two parts of the peripheral nervous system work together just like a car, sometimes you need the accelerator and other times the gas. When under stress sometimes we overuse the sympathetic nervous system, and it has the same effect as when you can’t take your foot off the gas pedal! Your system just gets over used and likely to get worn out much quicker. The solution is to put on the break by activating your parasympathetic nervous system. How can you do this?
1. Control your breathing.
This one trick can cheat the whole system. If you tell your body to slow your breathing, it has no choice but to relax. This is the first step in taking back control.
2. Keep an open mind and a sense of humor, and try to practice gratitude.
Having some confidence and the ability to laugh can help you get through a tough moment and maintain control of how you feel, no matter what anyone else does. Searching your mind for any positive that happened in the day actually trains your brain to focus less on the negative events and starts building your ability to experience some peace in any situation.
3. Stop with the unrealistic expectations.
The expectations we put on ourselves and others set us up for disappointment. First recognize that you have no control over someone else’s medical diagnosis and behavior. Walk away, let conflict pass and get back to breathing. Second, you are allowed to say no – to your family, to your friends and to yourself. Do only what you can comfortably fit into your schedule and energy level. If you think a task will take two hours, give yourself four and recognize it's the only thing you may do that day. Sometimes giving yourself permission to let go of how things “should be” and accepting them simply as they are can make all the difference in the world; bringing you peace in the middle of chaos.
Recommended readings “Why Zebras Don’t Get Ulcers” Robert Sapolsky; “The Happiness Advantage” Shawn Achor; “The Upward Spiral” Alex Korb. |
 |
Creativity Heals
Liz Kitchens |
I am a native born Floridian. I have endured more than my fair share of insults from smug, sometimes even cocky inhabitants of other states/countries. We have been criticized for our apparent lack of seasons, our proximity to amusement parks, our perceived inability to count election ballots, and for the inordinate number of amphibians and reptiles lurking along our shorelines. Sloughing off these slights, I’m here to boast about my community and the fact Central Florida is at the forefront of a movement within the health care industry, one involving creativity and wellness.
A couple of weeks ago I was lucky enough to spend time with fascinating people from arts organizations, caregiving agencies, colleges, philanthropic organizations and foundations, and national advocacy groups. Most of the participants (myself included) are ambassadors for a Creative Caregiving Initiative launched last year by the National Center for Creative Aging (NCCA). The Center developed an online Creative Caregiving Guide, the purpose of which is to create a community culture where arts and wellness are accessible to everyone. This kit, designed by master artists, contains creative modules intended to provide small moments of care and creativity for caregivers and their loved ones.
The focus is respite for the caregiver and quality of life for the patient. This was the brain-child of Margery Pabst Steinmetz, of the Pabst Foundation for the Arts. She says,
“The life of a caregiver is often filled with isolation, loneliness, stress, and depression with patches of sunlight and hope. We saw the arts as a beacon of hope.”
I admit to being a Margie Pabst groupie. Caregiving is her passion. Margie is a blogger; host of Caregivers Speak! a live online radio show; author- Enrich Your Caregiving Journey and Words of Care; and President of the National Center for Creative Aging. She believes creativity is at the crux of caregiving.
Margie is also on the Board of the Atlantic Center for the Arts. The Atlantic Center for the Arts is a totally cool artists-in-residence center nestled on a 70 acre ecological preserve in New Smyrna Beach, Florida. Even a single visit to this oasis can result in a drop in blood pressure it is so lovely and calming. Largely due to Margie’s influence, ACA has launched a Community Arts and Wellness Initiative focusing on connecting artists with patients and caregivers. I love the fact ACA is using the Creative Caregiving Guide to help all age demographics, from residents at the Ocean View Nursing and Rehab Center to homeless high school students.
Atlantic Center for the Arts
Arts and wellness programs are being introduced in medical schools at Harvard, Cornell, Columbia, and (thanks to Margie Pabst Steinmetz) at the University of Central Florida’s new medical school. They are finding that engagement with the arts is helpful in brain injuries, PTSD, and Alzheimer’s. Studies are finding emersion in the arts makes for better, happier and more empathetic doctors.
I have confessed in previous posts to being a creativity evangelist, so convinced am I of the potential life changing capabilities of creativity. I’m happy to have met Margie Pabst who is this description on steroids. She is proving that even a little creative thinking can have seismic changes in our community. |
 |
A Stepson Reconsiders
a Long-Held Resentment
Barry Jacobs |
A lot of blended families don’t really blend: the new “relatives” at first try to join together, but then they quietly distance themselves, however awkwardly, as differences and conflicts emerge, even as they try to pretend otherwise. My stepfather, Steve, and I made no such pretense—we were enemies from the start.
He entered my life when I was a cocky 16-year-old, about a year-and-a-half after the death of my own father from brain cancer. Steve was 45 at the time, and had already suffered a lifetime of tragedies, including the death of his mother when he was 6, 18 months of hard combat behind enemy lines in the Korean War, and the jolt of discovering his first wife in bed with another man. He was fixed up with my mother by mutual friends, latched onto her quickly, and held on tight, with no interest in dealing with her impudent children, especially the oldest son (me), who resembled the beloved husband for whom she still grieved.
I resented him from the moment I saw him. He was short and stocky; my dad had been tall. He was loud, opinionated, and boorish; my dad had taught me that only posers prattle on. He drank too much; my dad barely imbibed. For my mother’s sake, I spoke cordially to him, when I had to. But as we sidled past each other in the narrow hallways of the house, barely grunting acknowledgment, I saw an unwanted intruder with a hard, insolent stare. He saw a sneering, long-haired punk.
We might yet have found ways to bond. I loved riffing on my electric guitar, and he had a gifted musical ear, which allowed him to play any tune on the piano or banjo. He could fix anything, rewire the house, and put in new plumbing—skills I would’ve liked to have learned. But we remained caricatures to one another—usurping stepfather and disapproving stepson, Claudius and Hamlet. Even after I’d gone away to college and a productive adult life, tensions between us never eased. Greater distance helped us avoid overt conflict, nothing more.
On some level, I could see how my mother enjoyed caring for this moody, half-child man who could be both the joking, bragging life of the party and the needy, morose sulker in the corner. Steve worshipped her; she suckled him. When he turned 65 and insisted they retire and move to a South Florida gated community so he could play golf three times a week, she gave in, moving a thousand miles away from me and my growing family. To help him ward off his periodic depressions, she planned annual world excursions for them: Danube river cruise, African safari, Thai forest trek, Australian bush tour. For two decades, it seemed my most frequent communication with her was by postcard, with little contact with him. He was a curt voice on the phone before handing the receiver to my mom.
Then, as often happens when families enter the phase of late life, illness and reduced economic circumstances thrust us together to learn to relate differently. As he entered old age, Steve could no longer balance the checkbook, express himself intelligibly, or recall events. My mother long denied his progressing dementia—protectively speaking and remembering for him until eventually she took him to a neurologist for the dreaded diagnosis and futile meds. As his disease became worse and my mother became overwhelmed, I grew concerned about her health. Then she shocked me by calling me at work one day to ask me to send her $30,000 immediately to pay off debts. I’d been clueless that they’d lived too high for too long; their posh Florida condo and those exotic trips had cost them. Instead, I persuaded her to file for bankruptcy and, at my wife’s suggestion, for the two of them to move back up North to live in an apartment a mile from our Pennsylvania home so that we were near enough to help. We were now going to be a caregiving family.
I approached this change anxiously. We hadn’t lived in the same city for more than 25 years and didn’t know each other well. Even though what I knew of Steve I didn’t like, I still had the sense that caring for frail older adults was the right thing to do. I wanted my teenage children to learn that family value and I thought I owed my mother my help. Besides, having already written a book on caring for aging parents, I found it impossible to turn away from the challenge in real life.
The Steve who stepped off the plane in Philadelphia from Florida was a shrunken, weaker version of the man I first met.
His face was still cast in a mask of mild disdain, but his eyes now darted about uncertainly. As he walked, he shambled and swayed. On that first night, he tripped on the front step on the way into my house, hitting the paved walkway hard and ripping deep gashes in his thin, bony elbow and shin. As I quickly picked him up under his arms and propped him back on his feet, I could feel his ribs and how emaciated he’d become. He was light as a child. For the first time in my life, I had a feeling of sympathy for him, even admiration. He didn’t complain about pain or gape at his profusely bleeding wounds. While literally in the hands of his hated stepson and unable to hide his vulnerability, he still tried to maintain his dignity by keeping calm and holding his head up.
Life over the next year became organized by caregiving routines. My wife and I provided dinner for them three times a week, drove them to doctors’ appointments, picked up groceries. My mother fussed over and comforted Steve. Because he was no longer capable of stringing more than a few words together, Steve and I didn’t talk any more than we ever had, but his steady decline also peeled back his personality’s defenses—the Korean War vet gruffness, the smirks and condescension—exposing a raw, elemental openness. As I straightened up around their apartment or prepared lunch, I’d catch him watching me intently from his armchair with the wide-eyed, beseeching look of a curious 3-year-old. When I’d speak to him directly, he’d now smile back at me broadly with the rapt ardor of a puppy dog obeying the alpha male in a way I found both astonishing and disconcerting. The poles of our relationship had become unmoored. leaving me unsure whether this radical change was just an artifact of dementia or genuine gratitude.
Then things went rapidly downhill. Steve began wandering about the apartment at night in confusion while my mother slept too deeply. On several nights, he got out his toolkit and tinkered. One morning my mother woke to find he’d disconnected the faucets from the sinks and removed the metal protective plates from the electrical outlets. She feared he’d do something even more dangerous without 24-hour supervision. Though anguished and guilty, she decided to place him in a local nursing home.
I had mixed feelings about this. The part of me that was still invested in hating him thought, Just desserts. The bastard had it coming for a long time. But another part of me was softening toward him, wondering what this terrible diminishment must be like for him and what was going on in his failing mind. He’d lost so much in his life, then gained stability and comfort with my mother, only to now lose that, too. On my many visits to the nursing home, I’d watch him sitting at a table in the crowded and noisy day room of the dementia unit, staring blankly, getting thinner and more fog-bound with each passing month. His face—gaunt and impassive with numerous red sores and flaking skin—now prevented me from discerning his thoughts or emotions. To my surprise, that frustrated me. I couldn’t easily dismiss him as my damn stepdad; I felt sorry for him.
About two years after he’d moved to the nursing home, Steve died of sepsis due to bed sores. It was ironic to me that, of all the people in his 81 years of life, it was left to me, his most distant relation, to organize his funeral. On a hot July day, I led a group of 20 family members and friends on foot from the cemetery reception area to the plot where his ashes were to be buried. One by one, cousins and nieces stood at his graveside and told stories of how caring he was, how sensitive and attentive, how his humor lightened their lives. I stayed off to the side, feeling as wooden and hollow as the small, polished box of his cremains that I tightly held. Who was this man they were talking about? I didn’t know.
In the three years since, I can’t say I’ve actually grieved for Steve with any sadness or longing. Still, there’s a gnawing sense of having missed something important to my own identity. I’ve realized that for most of my adult life, I’ve thought of him as my foil, my anti-mentor, without really knowing the person against whom I pushed.
In the front closet in my mother’s apartment, I came across two dozen large photo albums of their exotic and expensive trips and began taking them down, one by one, to look at pictures of the life on the road he’d most enjoyed. In some, he looked young and virile and handsome—a good athlete, as my own father had been. In others, he beamed from some English castle tower, or struck a gallant pose on the Great Wall of China, or held my mother’s hand tenderly in some Italian square. I discovered that he was both well-organized and sentimental. The photos were put into the albums with great care and with labels of time and place handwritten in a steady, neat print. In some of the albums, I found he’d included trip diaries with enthusiastic and detailed descriptions he’d written of restaurants where they’d dined, sights they’d seen, and traveling American couples they’d befriended. These albums held no evidence of the aloof and disdainful man I’d experienced. Instead, here resided a big-hearted lover of life.
To my great surprise, the albums also included many photos of me and my wife and children at various places and times. They had the same neat labeling and care. Had he taken secret enjoyment in being with us, too?
So for nearly four decades, Steve and I knew—or didn’t know—each other, never advancing beyond the adversarial roles into which we first fell. Yes, I was and am the loyal protector of my father’s memory. But couldn’t I have still broken the ice with my stepfather? Why didn’t he? It’s only now, as the resentments that fueled our disconnection fade into the past, that I find myself embracing the process of trying to understand him and acknowledging the part of myself forever intertwined with him.
This blog is excerpted from "Intimate Enemies" by Barry Jacobs. The full version is available in the November/December 2016 issue, The Next Big Thing?: Psychotherapy and the Virtual Revolution.
|
| |
Caregivers Speak Blog:
Finding Your Inner Chutzpah!
By Bonnie Friedman |
Advocating for a loved one who is ill requires many things – time, attention and perseverance to start. Diplomacy and respect are other essential ingredients. But effective advocacy also requires a strong dose of chutzpah, that wonderful Yiddish word
blending personal guts and gumption. I have been advocating for my husband Bob for more than a quarter century through multiple hospitalizations and illnesses. One thing I have learned is that my role is as important as the doctors and nurses in ensuring he gets the best medical care. Acting on that knowledge means working with medical professionals as an equal, trusting my instincts and speaking up when I have questions or think something is wrong.
Lucky me! I was born with a chutzpah gene. But not everyone is so fortunate. Some are overwhelmed by the bureaucracy of a hospital or the complexity of our health care system. Others feel intimidated by medical professionals who speak in technical
terms that are hard to understand. Still others think doctors are gods who should not be questioned. But making sure your loved one gets the best medical care requires the full involvement and participation of a family member or very close friend, especially when the patient is hospitalized. Doctors are busy, often forced to practice medicine by the clock. Nurses are routinely overworked and understaffed. Health care can be fragmented, and electronic medical records are no substitute for good communication. One of the most important jobs of the advocate is connecting the dots – asking the right questions, paying attention to details and making sure that the entire medical team is on the same page. Taking up the charge requires confidence. That can start with basic research to better understand the patient’s condition and be poised to ask smart questions.
Keeping good notes and staying organized helps the advocate pay attention to details and follow up on questions or concerns. Doctors don’t always communicate well with one another, and nurses are sometimes left out of the loop. Issues can fall between the cracks, and misunderstandings can affect patient care. A well-informed advocate can help keep communication flowing. Advocates who are strong, persistent and professional get a better response from doctors too. Acting with diplomacy
and respect means you are more likely to receive them in return.
When you put it all together – education, organization and perseverance – confidence in your role as an advocate can grow. The more you do it, the better you get at it. Start by believing in yourself. Remember, you know the patient better than anyone else in the hospital.
Think about a time in your life when you felt confident about your role – perhaps at work or in a community or other organizational setting. Draw upon your strengths, life experiences, street smarts and common sense. You can apply that sense of assurance to your advocacy role. Practice asking questions or making your case in advance. If you’re still not feeling confident, be prepared to act the part, knowing even a shaky start is better than no start at all. Before you know it, you will have
some chutzpah of your own.
|
 |
The Caregiving Dilemma
By Elaine A. Malec, PhD |
For most families, there will come a time when one of the family members need help. Maybe it is as simple as picking them up from a medical procedure where they were told they can’t drive. Maybe, it is helping them move in to a new home. Helping family member is what families do. Helping is not something that changes the relationship, it’s part of being in a relationship. Except when it comes to caregiving.
Caregiving takes the primary role a person has in the family and requires it to change. For example, a daughter grows up with her mother being the “parent” and all the expectations that come with that role. A mother is the daughter’s role model (for better or worse) on what it means to be a woman and a spouse. As the daughter becomes an adult, the relationship between the mother and daughter becomes stressed as each tries to develop a healthy adult relationship with the other. This transition isn’t always smooth and it doesn’t end when the daughter turns 18 or even when she marries and has her own family. What happens when a daughter becomes the primary caregiver for her mother is the relationship dynamics stall out. Caregiving requires the daughter to limit how much she is willing to stress the relationship in order to gain her own independence and to get the validation from her mother that she is indeed a grown woman. A daughter must become her own person. She needs her mom to accept her as a separate person in order for the relationship to be fulfilling for both. How does a daughter insist that her mother treat her like an equal when her mother needs the daughter to be her caregiver? How does the daughter focus how to become her mother’s equal, when her mother is frail or ill? Instead of the mother and daughter continuing to work towards becoming equal adults in the relationship, the roles become reversed and the daughter becomes the mother, or at least takes on the role of providing care for her. In most cases, the role of caregiving becomes all consuming. The natural dynamics between mother and daughter are put aside and the focus is on how the daughter will fulfill the duties and responsibilities of caring for her mother’s growing needs.
In order for the mother and daughter to address this dilemma, they need to recognize the toll caregiving can take on their natural progression through this mother-daughter dynamic. They need to continue to have time together outside of the caregiving responsibilities. Keeping mutual interests up, whether it is conversation about gardening or going to the theater or watching a movie together, a mother-daughter relationship needs to be continually nurtured so both feel it is still satisfying. The daughter also needs to rely on her mother like good friends rely on each other. Often daughters who are caregivers do all the problem-solving and don’t feel it “right” to rely on their aging parent. However, this reluctance can rob the mother of feeling like she still has value.
Without a doubt, caregiving within a family can make a real change in the primary roles people play in a family. This change can prevent the natural evolution of these relationships and erode the health and meaning of them. However, there are ways to keep relationships from becoming one dimensional.
Check out
Elaine A. Malec, PhD on Margery's Radio Show - CLICK HERE
|
 |
Vanessa Jones Briscoe, PhD, MSN, ARNP
Department Chair, Aging Studies
Associate Professor
College of Health Sciences
Bethune-Cookman University
Daytona Beach, FL
briscoev@cookman.edu |
Hi my name is Vanessa and I have some exciting information to share; thanks to the National Center for Creative Aging (NCCA) initiative. I am the Department Chair of Aging Studies at Bethune-Cookman University (B-CU) located in Daytona Beach, FL. Our students graduate with a Bachelor of Science Degree in Aging Studies; and are compassionate and anxious to help older adults as they move into their career path of gerontology.
We started an intergeneration project; called Time-Out Respite Program (Time-Out). Students are matched with a hospice client to provide “companion care” and relieve the caregiver during their assigned visits. Time-Out had a positive impact on clients, caregivers and students. Students reported forming meaningful relationships with their families and noted better understanding of the strengths of older adults as well as the challenges they face at end-of-life. They (the students) were always seeking ways to engage their clients in meaningful activities.
Meanwhile, B-CU initiated another out-reach to educate Caregivers in our community. And as luck would have it, I became an Ambassador for the NCCA Creative Caregiving Guide (launched nationally in October, 2015). The NCCA Creative Caregiving Guide© is a FREE, web-based and community-shared resource specially designed for both family and professional caregivers of adults who live with Alzheimer's disease and related cognitive disorders. This tool (I thought) would be perfect for my students to interact with their clients in the Time-Out program and the Caregivers in our community. The leadership of the NCCA has agreed to help us put our plans into action at the stage play “Forget Me Not”. The performance is Saturday, May 14, 2016 at 2:00 pm. The play will be held at B-CU Performing Arts Center. For more information call 202-349-3803. Please join us for the kick-off and be prepared to have a “Good Time”!
|
Gary Glazner on the National Center for Creative Aging: Creative Caregiving Guide©
One of the projects that I am most proud of participating in is the National Center for Creative Aging (NCCA): Creative Caregiving Guide©. In conjunction with my interview on eCareDiary with Margery Pabst, who is a dear friend and the Board President of the NCCA, I want to look at the Creative Caregiving Guide© through the voice of a caregiver, the author Rebecca Solnit. A leading and well-loved non-fiction writer, she is probably best known for her essay “Men Explain Things to Me.”
Link to Creative Caregiving Guide©
http://creativecaregiving.creativeaging.org/
I am participating in a book club and we are reading on the theme of memory. I was intrigued when she introduces her mother, who is the first stages of memory loss, in the opening chapter of the “The Faraway Nearby.”
Solnit’s writing on dementia and her relationship with a loved one is among the best I have read. Anyone going through the caregiving experience with a parent, partner, friend, neighbor will benefit from reading, “The Faraway Nearby.”
“She became a geriatric delinquent, prone to lashing out and running away. We tried to forestall her solo expeditions by talking her on a long walk every morning through the pleasant residential streets with their burgeoning flower gardens. Then the rest of my conversations with her were chaotic or perilous, I talk to her mostly about the colors of the houses and about irises, honey-suckle, nasturtiums, passionflowers, sunflowers, morning glories, and the other plants we passed on those walks.”
You can almost feel the warmth a fragrance of the spring air filled with a blaze of color. Solnit does two things here that relate to using arts with a person navigating memory loss that are at the core of the Creative Caregiving Guide©. The first is she stays in the moment by focusing their discussion and attention on what is in front of her and her mother. Second she steps outside of their normal routine to spend time together on the walk.
The Creative Caregiving Guide© is about being in the moment and carving out a little time from the things we have to do each day when we are caring for each other.
For me as the founder and Executive Director of the Alzheimer’s Poetry Project I started jumping for joy when I read, “As I was writing this I went to see my mother, and a little way into trying to be with her in the era past when she would murmur more than an occasional word and I would only rarely understand it, I remembered that I had a copy of Rilke’s Dunino Elegies with me and read three of them to her. In one of them were the words, ‘what we’re now striving for was once/nearer and truer and attached to us/ with infinite tenderness. Here all is distance/ There it was breath… It was a good way to keep talking and I listened too, and the familiar lines became more fiercely elegiac, more stern and wild spoken aloud.”
Solnit gets to the heart of the Creative Caregiving Guide©, when she writes about using poetry as a good way to keep talking and how she also listened deeply to the words. All of the lessons in the Creative Caregiving Guide© are communication tools and a way to be together. For us to see, hear and listen deeply to each other.
|
|







